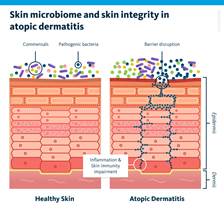
Atopic dermatitis (AD) is a chronic inflammatory skin condition marked by a weakened skin barrier. Two major contributors to this dysfunction are altered lipid composition and an imbalanced skin microbiome. While not the sole cause of AD, disruptions in both systems strongly influence disease severity.
Lipid alterations in AD
Healthy skin relies on a diverse mixture of lipids – especially ceramides – to maintain hydration and barrier integrity. In this study, tape‑strip samples from lesional, non‑lesional, and healthy skin were analyzed to assess the lipid composition in detail using shotgun lipidomics, a technique that enables broad and quantitative profiling of hundreds and thousands of lipid species.
Lesional AD skin showed:
- Higher total lipid levels, with cholesterol dominating lesional skin.
- Increased NS and NdS ceramides, which decline from lesional to non‑lesional to healthy skin. NS increases have been linked to psoriasis, while decreases relate to dry skin.
- Lower levels of barrier‑supporting ceramides (EOS, EOH), both essential for forming the lamellar lipid layers that prevent transepidermal water loss and protect against environmental stressors.
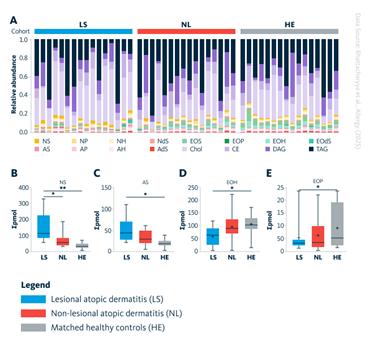
Overall lipid diversity increased along a gradient: lesional < non‑lesional < healthy skin.
Microbiome shifts and Staphylococcus imbalance
Further, microbial DNA was sequenced to characterize the community composition at the same sites. Microbial DNA sequencing of the samples demonstrated higher microbial abundance in AD, largely driven by Staphylococcus species.
Lesional skin showed:
- Strong overgrowth of Staphylococcus aureus, an inflammatory species.
- Reduced levels of beneficial commensals.
- A high ratio of inflammatory to protective Staphylococcus strains.
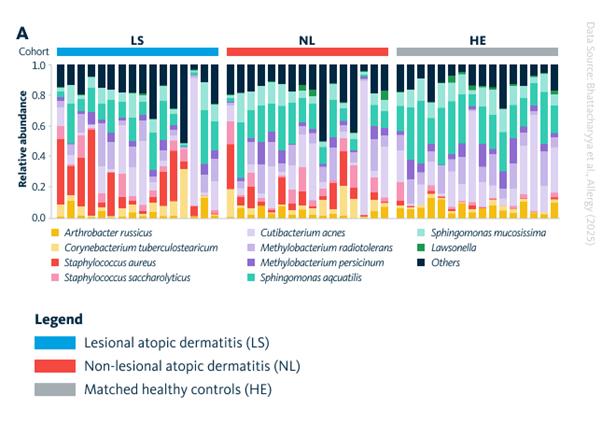
Staphylococcus hominis and other non‑pathogenic species were more common in non‑lesional and healthy skin.
Lipid-microbe interactions
Correlation network analyses revealed that healthy and non‑lesional skin have dense, interconnected lipid–microbe networks, whereas lesional skin is fragmented, dominated by isolated microbe‑centric modules.
Staphylococcus hominis emerged as particularly important. It negatively correlated with non-beneficial ceramides enriched in lesions.
Functional role of S. hominis
In addition, selected tape strips were used in culture‑based assays to explore how specific skin bacteria interact with lipids and other components collected from the skin surface. Using reconstructed human epidermis (RHE) models that mimic AD, researchers demonstrated that S. hominis can:
- Reduce lesion-enriched ceramide NdS 18:0;2/24:0;0.
- Improve epidermal structure.
- Shift lipid profiles toward a healthier state.
- Partially rescue inflammatory gene expression.
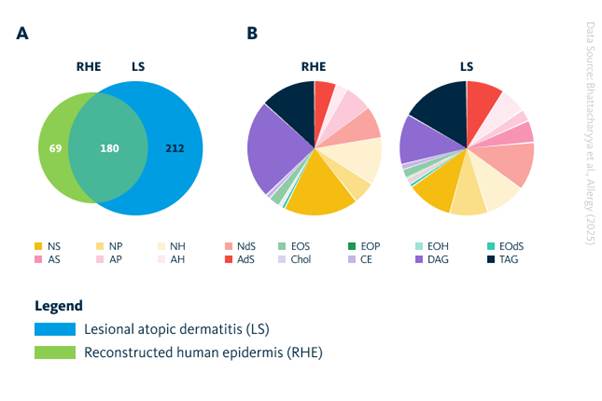
In patient data, increased S. hominis levels correlated with better barrier function, showing a clear negative association with transepidermal water loss.
Implications
These findings highlight S. hominis as a promising candidate for microbiome‑based therapies. They also underscore the value of integrating lipidomics with microbiome analyses to guide dermatology research, skin‑care product development, and claim support.
Lipotype Skin Lipidomics technology supports this work by providing high‑resolution lipid profiling for researchers, clinicians, and product developers.
Contact
Marta Vicini
Responsible account manager
service@lipotype.com






